Introduction
Hello and welcome back to our Colonoscopy Preparation Podcast series. I'm Bimal Maharjan, here once again to guide you step by step as you prepare for a colonoscopy. Leveraging my journey as a GI patient, this series aims to simplify and demystify the colonoscopy process for everyone involved.
Source of Information:
As always, our advice is anchored in the latest medical standards and guidelines provided by esteemed health organizations, combined with firsthand accounts and recommendations from gastroenterologists. Our goal is to blend professional guidance with personal insights to ensure you receive both scientifically sound and practically useful information.
Recall of Previous Episode:
Last time, we discussed the T-14 days before your colonoscopy, focusing on understanding and preparing your prep kit. We talked about how to pick the right prep kit tailored to your specific health needs, where to pick it up, and how to manage side effects that might arise during its use.
Connection and Series Overview:
Our podcast series is meticulously organized to guide you through every critical milestone leading up to your colonoscopy. Today, we're advancing to Episode 3, which zeroes in on the T-7 days mark—adjusting your medications and ensuring everything is lined up for the upcoming procedure.
Episode Outline:
In this episode, we’ll delve into the essential adjustments you need to make a week before your procedure. We'll cover everything from which prescription medications to continue or pause, to managing medications for specific conditions like heart or liver issues. We’ll also discuss how to ensure reliable transportation for the day of your colonoscopy.
Stay tuned, and by the end of this episode, you’ll be well-equipped to make informed decisions about your medications and have your logistics firmly in place. We’re here to help you navigate these adjustments smoothly, ensuring that you approach your colonoscopy day with confidence and peace of mind.
Medications
General:
Q1: Which prescription medications should I continue, and which should I pause before my colonoscopy?
As we get closer to your colonoscopy, one of the key preparations involves adjusting your prescription medications. Not all medications are the same, and the decision to continue or pause them isn’t one-size-fits-all. It's about understanding which medications can affect the procedure and how.
First, for anyone taking blood thinners—such as warfarin, clopidogrel, or even daily aspirin for heart health—it's typically necessary to pause these medications to reduce the risk of excessive bleeding during the procedure. Your doctor will give you specific instructions on when to stop taking these medications, often a few days before your colonoscopy.
Second, if you’re on diabetes medications, especially insulin or sulfonylureas that can lower your blood sugar, adjustments might be needed. Because you’ll be on a clear liquid diet before your procedure, there’s a risk your blood sugar could drop too low. Your healthcare provider might recommend reducing your dose or altering the timing of your medication.
Third, for medications related to blood pressure, heart conditions, or thyroid disorders, in most cases, you’ll continue taking these right up to the day of the procedure. However, always verify this with your doctor, as stability in blood pressure and heart rhythm is crucial.
For those on medications for mental health, such as antidepressants or antianxiety medications, these are generally continued to maintain emotional and psychological stability. Yet, it's important to discuss this with your healthcare provider, particularly how they might interact with anesthesia.
Guidelines from the American Society of Gastrointestinal Endoscopy and similar studies highlight the importance of medication adjustments to minimize risks during procedures. They provide protocols for managing medications in a way that balances procedure safety with ongoing health needs.
In summary, the key to managing your prescription medications before a colonoscopy is clear communication with your healthcare provider. They will guide you through which medications to pause, which to continue, and how to safely make these adjustments. By carefully managing your medications, you’re setting the stage for a successful and complication-free colonoscopy.
Heart Conditions:
Q2: How should I manage my medications for heart conditions such as hypertension or atrial fibrillation in preparation for the procedure?"
Managing heart condition medications as you prepare for a colonoscopy requires careful planning and consultation with your healthcare providers. Here’s what you need to consider:
Firstly, for hypertension medications, it’s generally recommended to continue these medications right up to the morning of your colonoscopy. The goal is to maintain stable blood pressure throughout the procedure, which helps prevent any cardiovascular complications. Common medications such as beta-blockers, ACE inhibitors, or calcium channel blockers should be taken as usual with a small sip of water even on the morning of your procedure.
Secondly, if you’re dealing with atrial fibrillation, particularly if you’re on blood thinners like warfarin or newer anticoagulants such as dabigatran or apixaban, the approach might be a bit different. These medications often require adjustments to minimize the risk of bleeding. Typically, your cardiologist may advise you to stop these medications a few days before the procedure, depending on your risk of stroke and the type of anticoagulant you’re using. This decision is crucial and should be made in coordination with your gastroenterologist and cardiologist.
Studies and guidelines, such as those from the American College of Cardiology, stress the importance of maintaining essential heart medications but adjusting anticoagulants under medical supervision to balance the risks of stroke against those of procedural bleeding.
References:
American College of Cardiology (ACC) guidelines on perioperative cardiovascular management for non-cardiac surgery can be found at American College of Cardiology.
Specific protocols for managing anticoagulants are detailed in the journal Circulation.
In conclusion, if you're managing a heart condition, the key takeaway is to never make changes to your cardiovascular medications without professional guidance. Always coordinate these adjustments with your cardiologist and gastroenterologist to ensure a safe and effective colonoscopy. Staying on top of your heart health is just as important as preparing your colon for the procedure.
Liver Conditions:
Q3: Are there any specific considerations for medications if I have liver conditions like cirrhosis or hepatitis?"
Dealing with a liver condition like cirrhosis or hepatitis adds an extra layer of complexity when you're preparing for a colonoscopy. It's critical to ensure that your liver can handle the medications involved both before and after the procedure.
For those of you navigating liver conditions, adjusting your medications before a colonoscopy involves several key considerations:
First, if you have cirrhosis, you need to be especially careful with medications that are metabolized by the liver. This includes many over-the-counter pain relievers such as acetaminophen, which, while generally safe in limited amounts, can be harmful in larger doses or when liver function is compromised. Your doctor might adjust the dosages or recommend alternatives that are safer for your liver.
Second, for conditions like hepatitis, you must also consider the impact of medications on your liver’s current state. Non-steroidal anti-inflammatory drugs (NSAIDs), which are often advised against before procedures due to their blood-thinning effects, can also cause liver damage if used inappropriately in patients with liver disease.
Third, it’s essential to review all medications, including herbal supplements and vitamins, with your healthcare provider. Some substances might exacerbate liver conditions or interact poorly with prescription medications you’re taking for liver health.
Research in the Journal of Hepatology suggests that patients with liver disease often require tailored medication plans to avoid exacerbating their condition. These plans are carefully crafted to minimize additional liver strain.
References:
Guidelines for managing liver patients undergoing surgery can be found in the Journal of Hepatology.
For safe medication use in liver disease, see resources provided by the American Association for the Study of Liver Diseases.
When preparing for a colonoscopy with a liver condition, the bottom line is to work closely with your gastroenterologist and possibly a hepatologist. They will guide you through safely adjusting your medications to protect your liver while ensuring the colonoscopy can be performed effectively. Remember, each step in adjusting your medications should be taken with an eye toward safeguarding your liver health.
Stomach Conditions:
Q4: Should adjustments be made to medications for acid reflux, ulcers, or other stomach conditions?
Preparing for a colonoscopy when you have stomach conditions such as acid reflux or ulcers adds another layer to your pre-procedure planning. It's vital to tailor your medication management to ensure your stomach remains as stable as possible.
Adjusting your stomach medications isn't just about comfort; it's about creating the safest environment for a successful colonoscopy.
For those dealing with stomach conditions, the approach to adjusting your medications needs careful consideration to avoid exacerbating your symptoms and to ensure the lining of your stomach is protected:
Firstly, if you're on proton pump inhibitors (PPIs) or H2 blockers for acid reflux or GERD, typically, you can continue these medications up to and including the day of your colonoscopy. These medications help maintain a stable stomach acid level, which is beneficial for reducing the risk of discomfort during fasting and the procedure itself.
Secondly, for those with ulcers, medications such as PPIs are also crucial in maintaining the protective lining of your stomach, which can help prevent bleeding. It’s usually recommended to continue these medications without interruption.
Third, if you are taking any antacids or alginate drugs like Gaviscon, you can generally continue these as needed up to the day before the procedure. However, it’s important to avoid any medications containing aluminum or magnesium within a certain time frame before the colonoscopy, as these can interfere with the visibility during the procedure.
Research indicates that maintaining anti-acid therapy in patients undergoing procedures can help minimize the risk of complications such as upper gastrointestinal bleeding, a concern particularly for patients with existing ulcers.
References:
For guidelines on managing gastroesophageal medications during endoscopic procedures, consult resources from the American Gastroenterological Association.
The effectiveness of continuing PPIs in preventing procedure-related complications is detailed in studies found in Gastroenterology.
In summary, if you’re managing stomach conditions like acid reflux or ulcers, it’s essential to continue your medications as prescribed to ensure the integrity of your stomach lining is maintained. Always discuss your specific medication regimen with your gastroenterologist as you prepare for your colonoscopy. Their guidance will ensure that your medications are optimized to support both your condition and the success of the procedure.
Diabetes (including weight loss medications like Ozempic):
Q5: What modifications are necessary for diabetes medications, including insulin and newer weight loss medications?"
Managing diabetes effectively requires careful attention to medication, and this becomes even more critical as you prepare for a colonoscopy. It’s like recalibrating your approach to ensure your blood sugar levels are stable and safe during the fasting required for the procedure.
Fine-tuning your diabetes medications isn't just tweaking numbers; it's about ensuring a balance that keeps you safe during your colonoscopy.
For those of you with diabetes, adjusting your medication regimen before a colonoscopy is essential to avoid both high and low blood sugar levels, which can complicate the procedure and your recovery.
Firstly, for insulin users, the key is to adjust your doses to compensate for the lower intake of food, especially while you are on a clear liquid diet the day before the procedure. Your healthcare provider might recommend reducing your insulin dose to prevent hypoglycemia. For example, if you use long-acting insulin, your dose may be decreased by as much as 20% to 50% the day before the colonoscopy.
Secondly, for those taking oral diabetes medications, such as metformin, you may need to adjust or even skip doses. This is particularly important since some of these medications, including metformin, can increase the risk of lactic acidosis if you become dehydrated during the prep.
Thirdly, regarding newer weight loss medications like Ozempic (semaglutide), which is also used to manage blood sugar levels in type 2 diabetes, you should consult with your healthcare provider. Typically, medications like Ozempic, which affect gastric motility and insulin secretion, may need to be paused temporarily to prevent gastrointestinal side effects and hypoglycemia during the fasting required for colonoscopy prep.
Clinical guidelines, such as those from the American Diabetes Association, highlight the importance of medication adjustments in patients undergoing fasting procedures to manage blood glucose levels effectively and prevent complications.
References:
American Diabetes Association’s guidelines on managing diabetes medications during fasting and procedures can be accessed at Diabetes Care.
To wrap up, if you’re managing diabetes, it's crucial to discuss your specific medications with your endocrinologist or diabetes specialist well before your colonoscopy. They can provide personalized advice on how to adjust your insulin and any other diabetes medications, ensuring you remain stable and safe throughout the procedure and recovery.
Kidney Conditions:
Q6: What adjustments should be made to my medications if I have kidney conditions such as chronic kidney disease (CKD) or are on dialysis?
Q7: Are there specific prep solutions that are safer or recommended for patients with kidney issues?
Dealing with kidney conditions such as chronic kidney disease or being on dialysis puts you in a special category that needs customized care, especially when it comes to preparing for a colonoscopy.
Firstly, regarding medication adjustments, if you have kidney disease or are on dialysis, many medications you might be taking for other conditions will need a second look. Medications that are cleared by the kidneys could build up in your body and potentially cause toxicity if not adjusted. For instance, certain blood pressure medications or diabetes medications may need to be reduced or skipped depending on your kidney function and dialysis schedule.
Secondly, concerning the prep solutions for the colonoscopy, it's crucial to avoid those that can be particularly harsh on the kidneys. Traditional osmotic laxatives that contain sodium phosphate should generally be avoided because they can significantly alter your electrolyte and fluid balance, which is dangerous for those with kidney issues. Instead, polyethylene glycol (PEG) solutions are often recommended because they are considered safer and less likely to affect kidney function or electrolyte balance.
Studies have shown that patients with kidney disease are at higher risk of electrolyte imbalances when using certain colonoscopy prep solutions. Therefore, guidelines suggest using non-phosphate based laxatives for these patients.
References:
Guidelines on safe prep solutions for patients with kidney disease can be found in the recommendations by the National Kidney Foundation, accessible at National Kidney Foundation.
Information on medication adjustments in patients with renal impairment can be reviewed in Clinical Kidney Journal.
In summary, if you're managing kidney conditions, make sure to consult closely with your nephrologist or renal specialist about which medications need adjustment and the safest prep solution for your colonoscopy. Tailoring these elements to your specific needs is key to ensuring a safe procedure and optimal outcomes.
Other Chronic Disease Conditions:
Autoimmune Disorders:
Q8: Should I make any changes to my medications for autoimmune conditions like rheumatoid arthritis or lupus?
Managing autoimmune conditions such as rheumatoid arthritis or lupus typically involves medications that can affect immune function and inflammation. It's crucial to consult with your rheumatologist or healthcare provider about these medications before a colonoscopy. Commonly, medications such as non-steroidal anti-inflammatory drugs (NSAIDs) might be paused due to their potential to affect bleeding. However, immunosuppressants like methotrexate or biologics may be continued based on your doctor's assessment of disease activity and overall health. The goal is to maintain disease control while minimizing procedure-related risks.
Respiratory Conditions:
Q9: How do I manage medications for asthma or COPD in preparation for my colonoscopy?
If you have asthma or COPD, maintaining optimal respiratory function is essential. You should continue using your inhalers and nebulizers as prescribed. However, if you're on oral corticosteroids or other systemic treatments, discuss with your pulmonologist whether any adjustments are needed. The key is to ensure that your respiratory condition is as stable as possible to avoid complications during the sedation and procedure. Your healthcare provider might also recommend a pre-procedure bronchodilator treatment if you are prone to bronchospasms.
Thyroid Disorders:
Q10: Are there considerations for my thyroid medications, especially if I have hypothyroidism or hyperthyroidism?
For patients with thyroid disorders, it's generally advised to continue thyroid medications like levothyroxine without interruption. These medications are critical to maintaining your metabolic balance and do not typically interfere with colonoscopy procedures. However, if you have concerns about your thyroid condition's stability, such as in cases of hyperthyroidism, consult with your endocrinologist. The focus should be on maintaining a stable thyroid function leading up to and during your procedure.
Mental Health Conditions:
Q11: Can I continue my psychiatric medications such as antidepressants, anti-anxiety meds, or mood stabilizers?
Specific Considerations for Chronic Conditions:
Q12: Are there supplements I should avoid due to my chronic disease(s), such as those that might interfere with medication efficacy or procedure safety?
Managing mental health is vital, and you should generally continue taking your psychiatric medications as prescribed, including antidepressants, anti-anxiety medications, and mood stabilizers. These medications help maintain your mental and emotional stability, which is particularly important when facing a medical procedure. However, because some psychiatric medications can interact with anesthesia, it's important to discuss all the medications you are taking with your gastroenterologist and anesthesiologist. They may make specific recommendations or adjustments to ensure your safety during the procedure.
Supplements
Vitamins:
Q13: Which vitamins are safe to continue, and which should be stopped, particularly those that might affect bleeding or healing?
When preparing for a colonoscopy, it’s important to consider how certain vitamins might interact with bleeding and healing processes:
Vitamin K:
Guidance: Vitamin K plays a crucial role in blood clotting. Generally, it's safe to continue taking vitamin K as part of a multivitamin or in your diet unless you are taking blood thinners like warfarin. In such cases, keep your vitamin K intake consistent to avoid interfering with medication effectiveness.
Vitamin E:
Guidance: Vitamin E has natural blood-thinning properties. It is usually recommended to stop taking high-dose vitamin E supplements a week before your procedure to reduce the risk of excessive bleeding. However, the small amounts in multivitamins or diet are typically not a concern.
Omega-3 Fatty Acids (Fish Oil):
Guidance: Like vitamin E, omega-3 supplements, often taken for heart health, can thin the blood. It’s advised to stop taking these supplements 7-10 days before your colonoscopy to minimize bleeding risks.
Iron Supplements:
Guidance: Iron supplements are often stopped several days before a colonoscopy because they can darken the lining of the colon, potentially obscuring the view during the procedure. This is particularly important if you're being evaluated for sources of bleeding in the intestine.
Herbal Supplements:
Guidance: Many herbal supplements, including but not limited to garlic, ginkgo biloba, and ginger, have blood-thinning properties. It’s best to discontinue these types of supplements at least a week before your procedure to avoid any increased risk of bleeding.
Research and guidelines suggest that minimizing supplements with anticoagulant properties can help reduce the risk of bleeding during procedures that involve mucosal surfaces, such as a colonoscopy.
References:
You can find more detailed guidelines and studies on the impact of dietary supplements on surgical procedures from sources like the American Society of Anesthesiologists, available online at ASA - American Society of Anesthesiologists.
Maintaining a balance in your vitamin intake is key as you prepare for a colonoscopy. While some vitamins are essential and safe to continue, others, especially those with anticoagulant properties, should be paused. Always discuss your specific supplements and dietary habits with your healthcare provider to tailor your preparation safely and effectively. This careful planning ensures that you are in the best possible condition for your colonoscopy, minimizing any risks associated with bleeding or visibility during the procedure.
Probiotics, Fibers, Prebiotics, Synbiotics:
Q14: Should I pause probiotics or any fiber supplements prior to my colonoscopy, and if so, when?
A: When gearing up for a colonoscopy, adjusting your intake of dietary supplements that affect digestive health, such as probiotics, fibers, prebiotics, and synbiotics, is important for a few reasons:
Fiber Supplements:
Guidance: Fiber supplements, especially those containing bulk-forming agents like psyllium, should be paused before your colonoscopy. These supplements can interfere with the bowel cleansing process by creating residue that coats the colon walls, potentially obscuring visibility during the procedure.
Timing: It is typically recommended to stop taking fiber supplements at least 5 to 7 days before your procedure to ensure that your colon is clear.
Probiotics:
Guidance: Probiotics are generally considered safe to continue, as they do not affect the clarity of the colon. However, since they are meant to populate the gut with beneficial bacteria, their effects can be negated by the bowel cleansing needed for a colonoscopy. Therefore, some healthcare providers might recommend pausing them a few days before the procedure.
Timing: If advised by your doctor, stop taking probiotics 3-4 days prior to your colonoscopy.
Prebiotics and Synbiotics:
Guidance: Like probiotics, prebiotics and synbiotics are used to enhance gut health. Since these can also contribute to residue in the colon, it might be suggested to pause them along with fiber supplements.
Timing: Stopping prebiotics and synbiotics should align with stopping fiber supplements—about 5 to 7 days before your colonoscopy.
Studies indicate that a clear, residue-free colon is crucial for effective colonoscopy procedures. Fibers, especially insoluble types, can hinder this by remaining in the colon despite cleansing efforts.
References:
The American Society for Gastrointestinal Endoscopy provides guidelines on dietary restrictions before a colonoscopy, which include recommendations on fiber and supplement intake. These can be accessed online for detailed guidance.
In summary, while supplements like probiotics may not necessarily need to be paused, fiber supplements, prebiotics, and synbiotics should be discontinued several days before your colonoscopy to ensure a thorough and effective bowel cleanse. Always check with your healthcare provider for personalized advice based on your specific health needs and the types of supplements you're taking. Properly managing these supplements will help ensure that your colonoscopy goes smoothly, providing your doctor with a clear view of your colon.
Herbs and Spices
General:
Q15: Are there herbs or spices I should avoid due to their potential impact on blood clotting or hydration levels?
When preparing for a colonoscopy, it's important to consider the effects of certain herbs and spices that might influence blood clotting or hydration:
Blood Clotting: Some herbs have natural anticoagulant properties, which can increase the risk of bleeding. Notably, herbs like garlic, ginkgo, and ginseng should be avoided as they can thin the blood. It's recommended to stop using these herbs at least one week before your procedure to ensure they don't complicate the process by increasing bleeding risks.
Hydration Levels: Spices such as cayenne pepper, which might cause diuresis or mild dehydration, should be used cautiously. While they generally do not need to be completely avoided, it's wise not to consume them in large quantities before your procedure to maintain optimal hydration.
Specific Herbs (Ashwagandha, Turmeric, Ginger, etc.):
Q16: Do common supplements like ashwagandha, turmeric, or ginger need to be discontinued, and what are the reasons?
Addressing common supplements:
Ashwagandha: This supplement is generally recognized for its adaptogenic properties and doesn't significantly affect blood clotting or hydration. However, because it can interact with other medications and potentially influence blood pressure and sugar levels, it's prudent to discuss with your healthcare provider whether to continue or pause it as your colonoscopy approaches.
Turmeric: Known for its anti-inflammatory properties, turmeric can also thin the blood due to its curcumin content. If you're taking turmeric supplements, particularly in high doses, it's advisable to discontinue their use about a week before your colonoscopy to prevent any potential increase in bleeding risk.
Ginger: While ginger is beneficial for digestion and nausea, it also has mild blood-thinning effects. If you're using ginger supplements, consider stopping them a few days before the procedure to avoid exacerbating any bleeding issues.
Studies suggest that herbal supplements with anticoagulant properties can pose risks during surgical procedures by increasing bleeding. Therefore, managing their intake before medical procedures like a colonoscopy is crucial.
References:
Comprehensive guidelines on the perioperative management of medications, including herbal supplements, can be found on the American Society of Anesthesiologists website at American Society of Anesthesiologists.
In summary, while herbs and spices are commonly used for their health benefits, their impact on blood clotting and hydration can be significant when preparing for a colonoscopy. It's essential to evaluate your use of these supplements and discuss them with your healthcare provider. Stopping herbs that affect blood clotting, like turmeric and ginger, at least a week before your procedure, and moderating the use of others that can impact hydration, will help ensure a safe and effective colonoscopy
Allergy Medications
General:
Q17: Can I continue taking my routine allergy medications, or are there any that might interfere with the procedure or anesthesia?"
Most routine allergy medications, including antihistamines and steroid nasal sprays, can be continued as they generally do not interfere with anesthesia or the colonoscopy procedure itself. However, it's important to discuss all medications, including over-the-counter allergy remedies, with your healthcare provider. Some antihistamines can cause drowsiness or interact with sedatives used during the procedure, so your doctor may recommend adjusting the timing of your doses.
NSAIDs and Painkillers
General:
Q18: Which NSAIDs and painkillers should I avoid due to their blood-thinning properties, and when should I stop taking them?
Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, naproxen, and aspirin, should generally be avoided before a colonoscopy due to their blood-thinning effects, which can increase the risk of bleeding. It is typically recommended to stop taking these medications 5 to 7 days before the procedure. If you need pain relief during this period, acetaminophen (Tylenol) is a safer alternative as it does not have the same blood-thinning properties.
Additional Concerns for Chronic Diseases
Managing Flares or Symptoms:
19: What precautions should I take if my chronic condition flares up during the preparation period?
If you have a chronic condition that flares up during your preparation for a colonoscopy, it's crucial to contact your healthcare provider immediately. They may need to adjust your medications or take other steps to manage your symptoms safely. It's also important to maintain hydration, especially if your preparation involves bowel cleansing, which can be dehydrating.
Emergency Contact:
Q20: Should I provide information about my chronic conditions to the medical team in case of an emergency during the procedure?
Absolutely. It is essential to inform the medical team conducting your colonoscopy about all chronic conditions you have. Provide a detailed medical history and a list of all medications you're taking, including dosages and schedules. This information can be crucial in managing any complications or emergencies that might arise during the procedure.
Q21: Should I stop smoking, drinking alcohol?
Yes, it's advisable to stop smoking and refrain from drinking alcohol at least 24 hours before your colonoscopy. Smoking can affect blood flow and wound healing, while alcohol can interfere with anesthesia and increase the risk of bleeding. Stopping both can help ensure a safer and more effective procedure.
Transportation and Support
Q22: How long after the procedure will I need someone to be with me?
After a colonoscopy, it is essential that you have someone with you for at least 24 hours. The sedatives used during the procedure can impair your judgment, coordination, and reaction times, making it unsafe for you to drive or operate machinery. Additionally, having someone nearby is important in case there are complications or if you experience adverse effects from the anesthesia.
Q23: Can the person driving me wait at the facility, or will they need to come back to pick me up?
This can vary by facility, but generally, the person driving you can wait at the facility if they prefer. Some facilities have lounges or waiting areas for drivers. However, due to space or policy limitations, they might be asked to return later. Check with your specific facility beforehand to understand their policies.
Q24: What arrangements should I make for my ride home if I'm using a ride service or public transportation?
If you're planning to use a ride service or public transportation, it's advised to arrange this in advance. Ensure that the service is available at the time you're likely to be discharged, and inform them that you will be recovering from sedation. It's best, however, to be accompanied by a friend or family member even if using these services, as you may still be feeling the effects of the anesthesia.
Q25: Are there services available through the hospital or clinic to assist with transportation if I can't find a driver?
Many hospitals and clinics can help arrange transportation for patients who do not have a driver. Contact the facility ahead of your procedure to inquire about these services. They may be able to provide or suggest local options that ensure you get home safely
Q26: What instructions or information will my driver or accompanying adult need to know on the day of the procedure?
Your driver or accompanying adult should know the details about the timing of the procedure, estimated duration, and discharge procedures. They should have contact information for the medical facility and understand that you may need assistance getting home due to the sedation. Additionally, they should be prepared to monitor your recovery immediately after the procedure for any signs of complications.
General Pre-Procedure Preparations
27: Should I prepare any documents or medical information to bring with me on the day of the procedure?
Yes, you should bring a list of all medications you are currently taking (including supplements), any relevant medical history documents, and your health insurance information. Also, bring any referral notes or instructions from your doctor.
Q28: How should I dress for the procedure, and are there any items I should bring for comfort or necessity?
Dress in loose, comfortable clothing that is easy to remove and put on. You will likely be asked to change into a hospital gown for the procedure. It’s also a good idea to bring a list of your current medications, a small blanket or throw if you tend to get cold easily, and a book or magazine for any waiting periods. Avoid bringing valuables or jewelry.
Conclusion
As we wrap up today’s episode, I want to thank you for joining me on this important journey through your T-7 day preparations for your upcoming colonoscopy. We’ve covered a lot today, from how to adjust your medications safely to ensuring you have the right support and transportation arrangements in place. It’s all about making sure you’re as prepared as possible, reducing stress, and minimizing any risks during your procedure.
We discussed the critical adjustments for various chronic conditions and how to handle medications that can impact your procedure outcome. Remember, the key takeaway from today is communication — keep in close contact with your healthcare providers about any changes in your condition or concerns you might have as your procedure date approaches. Your safety and comfort are paramount, and proper preparation can make all the difference.
Looking ahead, in our next episode, we'll move even closer to your procedure day, focusing on the T-5 days mark. We'll dive into specific dietary adjustments, what you should expect in the final days leading up to your colonoscopy, and how to manage last-minute anxieties or concerns. Stay with us as we continue to guide you through each step of your colonoscopy preparation.
Thank you for your trust and attention. Here’s to a smooth and successful colonoscopy. See you next time!
T-7 Days Colonoscopy Preparation User Guide
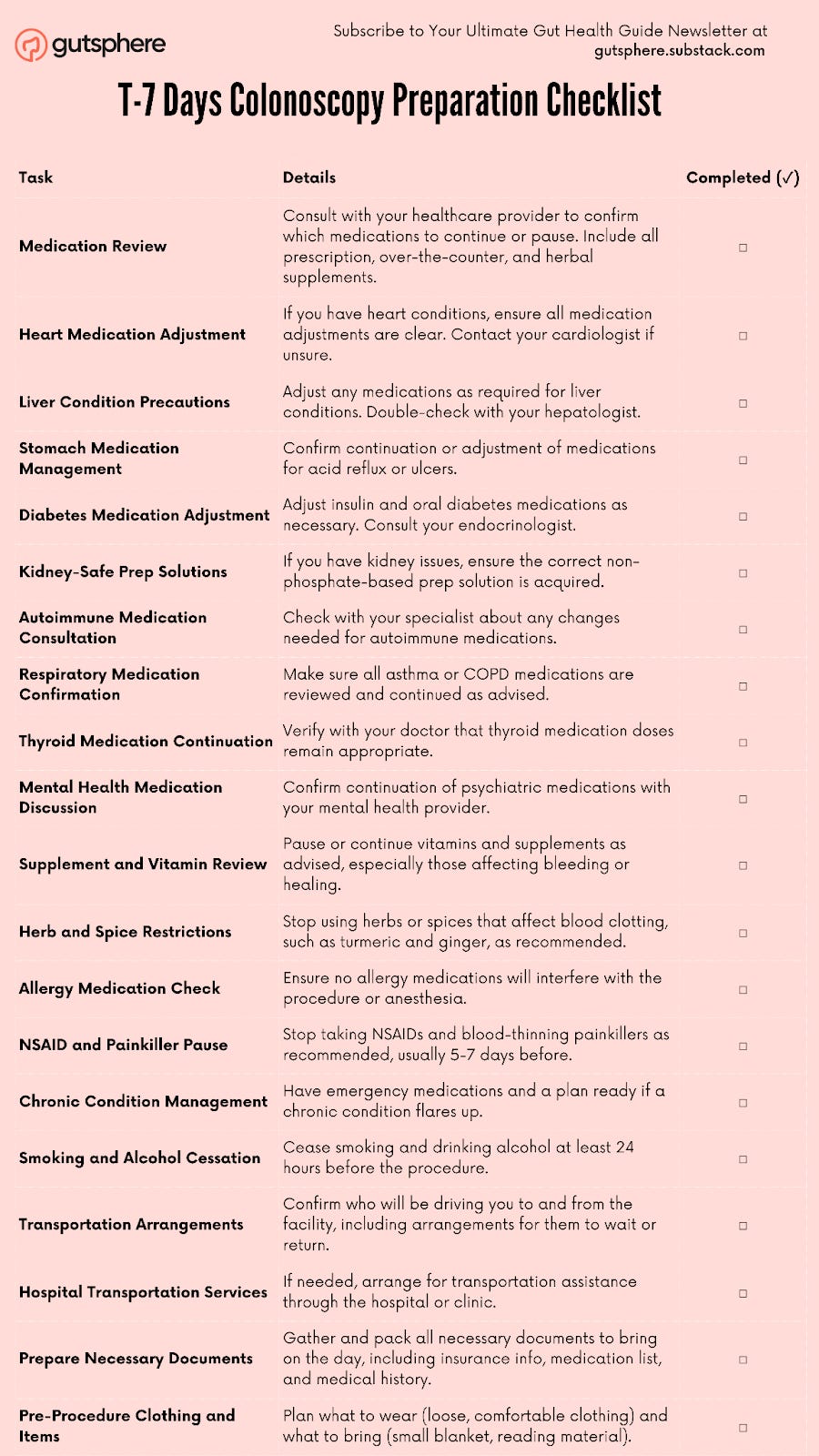
T-7 Days Colonoscopy Preparation Checklist
Request
Share
Our sincere request to you is to share the newsletter with your friends, family, and community so that they can benefit from the content. Also it will help us grow the newsletter, and eventually, as we release more content, digital tools, and more we will enable people around the world to live chronic disease free.
Subscribe
Feedback
Also, please give us feedback so that we can improve the content. And if there are any topics that you want us to cover please send us your questions and topics. Furthermore, if you try any of the things we provided information please share your experience with us.
Thank You
GutSphere Team
Disclaimer
Please note that the information provided in this newsletter is for informational purposes only and should not be considered as a substitute for professional medical advice, diagnosis, or treatment. If you have any concerns or questions about our health, please consult with a licensed healthcare professional. The information contained in this newsletter is not intended to diagnose, treat, cure, or prevent any disease. The publisher and authors of this newsletter assume no responsibility for any adverse effects that may result from the use of the information contained herein.
References:
Medications General:
Heart Conditions:
Liver Conditions:
Stomach Conditions:
Diabetes (including weight loss medications like Ozempic):
Kidney Conditions:
Autoimmune Disorders:
Respiratory Conditions:
Thyroid Disorders:
Mental Health Conditions:
Vitamins:
Probiotics, Fibers, Prebiotics, Synbiotics:
Herbs and Spices General:
Specific Herbs (Ashwagandha, Turmeric, Ginger, etc.):
Allergy Medications General:
NSAIDs and Painkillers General:
Additional Concerns for Chronic Diseases:
Transportation and Support:
General Pre-Procedure Preparations: